Torsades de Pointes, a term derived from the French phrase “twisting of the points,” is a specific type of life-threatening ventricular tachycardia. This condition, characterized by its unique appearance on the electrocardiogram (ECG), is a dance of the heart that no one wishes to experience. A rapid, irregular heart rhythm can lead to sudden cardiac death if not promptly treated.
The heart, a muscular organ that pumps blood throughout the body, relies on a complex electrical system to function correctly. When this system goes awry, arrhythmias or abnormal heart rhythms can develop. Torsades de Pointes is one such arrhythmia, and its understanding is crucial for medical professionals and patients.
Chapter 1: Introduction to Torsades de Pointes
- The heart’s rhythm is a delicate balance of electrical impulses. When these impulses are disrupted, the heart can beat too fast, slow, or irregularly. Torsades de Pointes (TdP) is one such disruption, a unique and dangerous form of ventricular tachycardia.
- At its core, TdP is a rapid heart rhythm originating from the heart’s lower chambers, the ventricles. What sets TdP apart from other forms of ventricular tachycardia is its appearance on the ECG. The heart rate during a TdP episode can exceed 250 beats per minute, and the QRS complexes—representative of the ventricular activity—appear to twist around an imaginary baseline.
- The significance of understanding TdP extends beyond its unique ECG appearance. This arrhythmia can degenerate into ventricular fibrillation, a chaotic rhythm leading to sudden cardiac death. Recognizing and treating TdP promptly is, therefore, of utmost importance.
- While TdP is relatively rare, certain factors increase its risk. These include specific medications, electrolyte imbalances, and genetic conditions like Long QT Syndrome. Throughout this book, we will delve deeper into these risk factors, ensuring a thorough understanding of the condition.
Chapter 2: The Anatomy of the Heart: A Brief Overview
The heart, often described as the body’s engine, is a muscular organ in the chest’s centre. Comprising four chambers—two atria and two ventricles—it pumps oxygen-rich blood to various body parts and receives oxygen-depleted blood in return.
For the heart to function efficiently, a synchronized contraction of its chambers is essential. This synchronization is achieved through a complex electrical system. The sinoatrial (SA) node in the right atrium generates an electrical impulse that travels through the atria, causing them to contract and push blood into the ventricles.
This impulse then reaches the atrioventricular (AV) node, a small cell cluster between the atria and ventricles. After a brief pause, the AV node sends the impulse down the Bundle of His and into the Purkinje fibres, resulting in the ventricles contracting and pumping blood out of the heart.
Any disruption in this electrical pathway can lead to arrhythmias. In the subsequent chapters, we will explore how Torsades de Pointes fits into this picture and the electrical anomalies that give rise to it.
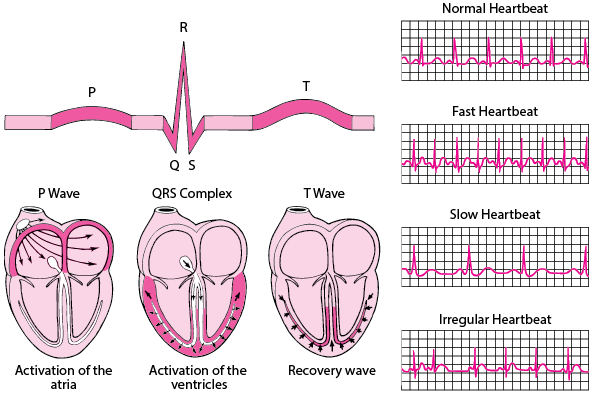
An electrocardiogram (ECG) represents the electrical current moving through the heart during a heartbeat. The current’s movement is divided into parts, and each part is given an alphabetic designation in the ECG.
Chapter 3: Electrical Conduction and Arrhythmias
The heart’s electrical system is a marvel of nature. It ensures that the heart beats in a coordinated and rhythmic manner, supplying blood to every body part. However, when this system malfunctions, it can lead to arrhythmias or abnormal heart rhythms.
The Electrical Pathway
As mentioned in the previous chapter, the heart’s electrical journey begins at the sinoatrial (SA) node, often called the heart’s natural pacemaker. This node fires an electrical impulse that travels through the atria, causing them to contract and push blood into the ventricles.
The impulse then reaches the atrioventricular (AV) node, pausing briefly. This pause allows the ventricles to fill with blood. The AV node then transmits the impulse down the Bundle of His, which divides into the left and right bundle branches. These branches further split into the Purkinje fibres, which spread the inspiration throughout the ventricles, causing them to contract.
Arrhythmias: When Things Go Awry
An arrhythmia occurs when there’s a disruption in the heart’s electrical system. This can be due to various reasons, including:
- Ectopic Beats: These are extra heartbeats that originate outside the SA node. They can occur in the atria, the AV node, or the ventricles.
- Reentry: This happens when an electrical impulse gets “stuck” in a loop, causing the heart to beat faster than usual. This is the mechanism behind many tachycardias, including Torsades de Pointes.
- Blocked Impulses: Sometimes, the electrical impulse can get partially or entirely blocked. This can lead to bradycardia (slow heart rate) or a complete cessation of the heart’s electrical activity.
Torsades de Pointes: A Unique Arrhythmia
Torsades de Pointes is a form of polymorphic ventricular tachycardia. Its association with a prolonged QT interval on the ECG makes it unique. The QT interval represents the time it takes for the heart’s ventricles to depolarize and then repolarize. When this interval is prolonged, it can set the stage for TdP.
In the following chapters, we’ll delve deeper into the causes and risk factors of Torsades de Pointes, its clinical presentation, and the intricacies of its diagnosis and treatment.
Chapter 4: Causes and Risk Factors of Torsades de Pointes
Understanding the causes and risk factors of Torsades de Pointes is crucial for both prevention and management. While some individuals might have a genetic predisposition, others might develop TdP due to external factors.
- 1. Medications: Numerous drugs can prolong the QT interval, increasing the risk of TdP. These include certain antibiotics, antipsychotics, and antiarrhythmic drugs. Healthcare professionals need to be aware of these medications and monitor patients accordingly.
- 2. Electrolyte Imbalances: Abnormal potassium, magnesium, and calcium levels can affect the heart’s electrical activity. Low potassium (hypokalemia) and magnesium (hypomagnesemia) are particularly associated with a heightened risk of TdP.
- 3. Genetic Factors: Long QT Syndrome (LQTS) is a genetic condition that predisposes individuals to prolonged QT intervals and TdP. There are various types of LQTS, each associated with specific genetic mutations.
- 4. Other Medical Conditions: Certain conditions, such as bradycardia (slow heart rate), heart failure, and myocardial infarction (heart attack), can increase the risk of TdP.
- 5. Alcohol and Substance Abuse: Chronic alcoholism and the use of specific recreational drugs can lead to electrolyte imbalances and other cardiac complications, increasing the risk of TdP.
- 6. Hormonal Factors: Some studies suggest that women might be at a higher risk of drug-induced TdP, especially during specific periods of their menstrual cycle.
Chapter 5: Clinical Presentation and Diagnosis
Patients’ clinical presentation can vary significantly when Torsades de Pointes (TdP) strikes. Some may experience alarming symptoms, while others remain asymptomatic until a life-threatening event occurs.
Symptoms of Torsades de Pointes
- Palpitations: The most common symptom, palpitations, are sensations where one feels their heart is racing, pounding, or fluttering.
- Dizziness or Lightheadedness: Patients might feel dizzy or lightheaded due to the rapid heart rate and reduced cardiac output.
- Syncope: Some patients might experience a sudden and temporary loss of consciousness, often described as “fainting.”
- Seizures: In rare cases, the reduced blood flow to the brain can trigger seizures.
- Cardiac Arrest: If TdP degenerates into ventricular fibrillation, it can lead to cardiac arrest, where the heart stops beating entirely.
Diagnosing Torsades de Pointes
The diagnosis of TdP is primarily based on the electrocardiogram (ECG). However, a thorough medical history and physical examination are also crucial.
- Electrocardiogram (ECG): The hallmark of TdP on an ECG is a twisting pattern of the QRS complex around the isoelectric line, with a varying amplitude and axis. Additionally, a prolonged QT interval often precedes the onset of TdP.
- Medical History: It’s essential to gather information about the patient’s medications, especially those that prolong the QT interval. A family history of sudden cardiac death or known genetic conditions like Long QT Syndrome can provide valuable clues.
- Blood Tests: These can help identify electrolyte imbalances, such as low potassium or magnesium levels, which might increase the risk of TdP.
- Holter Monitor: For patients who experience sporadic symptoms, a portable ECG device worn for 24 to 48 hours can help capture abnormal heart rhythms.
Chapter 6: The ECG: Recognizing Torsades de Pointes
The electrocardiogram (ECG) is a vital tool in diagnosing TdP. It visually represents the heart’s electrical activity, allowing clinicians to identify and interpret abnormalities.
Understanding the ECG
An ECG trace consists of various waves and intervals:
- P wave: Represents atrial depolarization.
- QRS complex: Represents ventricular depolarization.
- T wave: Represents ventricular repolarization.
- QT interval: The time from the start of the QRS complex to the end of the T wave, representing the total time taken for ventricular depolarization and repolarization.
Recognizing Torsades de Pointes
- The characteristic feature of TdP on an ECG is the twisting of the QRS complex around the isoelectric line. This “twisting” appearance gives TdP its name, which translates to “twisting of the points.” The amplitude and axis of the QRS complex vary, creating a sine-wave impression.
- Another crucial feature is the prolonged QT interval, which often precedes TdP. A prolonged QT suggests that the heart muscle takes longer than usual to recharge between beats, setting the stage for this dangerous arrhythmia.
Chapter 7: Treatment and Management Strategies
Immediate intervention is crucial when TdP occurs, as it can quickly degenerate into ventricular fibrillation, leading to cardiac arrest.
Acute Management
- Immediate Defibrillation: Rapid defibrillation is necessary if the patient is unconscious or shows signs of reduced cardiac output.
- Magnesium Sulfate: Even if magnesium levels are standard, intravenous magnesium sulfate is the drug of choice for TdP. It helps stabilize the heart’s electrical activity.
- Temporary Pacing: If TdP recurs despite magnesium therapy, overdrive pacing using a temporary pacemaker can suppress the arrhythmia.
Long-term Management
- Avoidance of QT-Prolonging Drugs: Patients diagnosed with TdP should avoid medications that prolong the QT interval.
- Correction of Electrolyte Imbalances: Regular monitoring and correcting potassium and magnesium levels are essential.
- Beta-blockers: These drugs can help reduce the occurrence of TdP in patients with Long QT Syndrome.
- Implantable Cardioverter-Defibrillator (ICD): For high-risk patients, an ICD can detect life-threatening arrhythmias and deliver a shock to restore normal rhythm.
Chapter 8: Drugs and Medications: What to Avoid
The relationship between certain drugs and Torsades de Pointes (TdP) is well-established. Many medications, spanning various therapeutic classes, can prolong the QT interval and predispose individuals to this dangerous arrhythmia.
- 1. Antiarrhythmics: Ironically, some drugs meant to treat heart rhythm disorders can cause TdP. Examples include quinidine, procainamide, and sotalol.
- 2. Antibiotics: Certain antibiotics, especially macrolides like erythromycin and fluoroquinolones like ciprofloxacin, have been linked to QT prolongation.
- 3. Antipsychotics: Drugs like haloperidol, risperidone, and ziprasidone, often used to treat mental health disorders, can prolong the QT interval.
- 4. Antidepressants: Some antidepressants, such as citalopram and amitriptyline, have been associated with a risk of TdP.
- 5. Antiemetics: Medications like ondansetron, used to prevent nausea and vomiting, can affect the QT interval.
- 6. Diuretics: While not directly causing QT prolongation, diuretics can lead to potassium loss, indirectly increasing TdP risk.
Patients should always consult their healthcare provider before starting or stopping any medication. Regular monitoring, including periodic ECGs, is crucial for those on drugs known to affect the QT interval.
Chapter 9: Long QT Syndrome and Its Connection
Long QT Syndrome (LQTS) is a genetic disorder predisposing individuals to prolonged QT intervals and TdP. Understanding LQTS is crucial, as it’s one of the primary risk factors for TdP.
Types of LQTS
There are several types of LQTS, each associated with specific genetic mutations. The three most common are:
- LQT1: Caused by a mutation in the KCNQ1 gene. It’s the most common type and is often triggered by physical exertion.
- LQT2: Resulting from a mutation in the KCNH2 gene. Emotional stress or sudden loud noises often trigger it.
- LQT3: Caused by a mutation in the SCN5A gene. It’s less common and can occur during rest or sleep.
Diagnosis and Management
Diagnosing LQTS involves a combination of ECG, genetic testing, and a thorough family history. Management strategies include beta-blockers, lifestyle modifications, and potentially an implantable cardioverter-defibrillator (ICD) for high-risk individuals.
Chapter 10: Complications and Prognosis
- If not promptly treated, Torsades de Pointes can lead to several complications, the most severe being ventricular fibrillation and sudden cardiac death. Other potential complications include heart failure, stroke, and cognitive impairments due to reduced blood flow to the brain.
- The prognosis for TdP varies. The forecast is generally favourable if the underlying cause is identified and addressed—like discontinuing a QT-prolonging drug or correcting an electrolyte imbalance. However, the risk remains for those with genetic predispositions like LQTS, necessitating ongoing monitoring and management.
Chapter 11: Prevention and Lifestyle Modifications
Preventing Torsades de Pointes (TdP) is paramount, especially for those at increased risk. While some factors, like genetics, cannot be changed, many preventive measures can be taken to reduce the likelihood of this arrhythmia.
- 1. Medication Awareness: Always consult a healthcare provider before starting or stopping any medication. Regular monitoring, including periodic ECGs, is essential if on a drug that prolongs the QT interval.
- 2. Maintain Electrolyte Balance: Ensure a balanced potassium and magnesium intake. Foods rich in these minerals include bananas, spinach, nuts, and whole grains. Avoid excessive alcohol consumption, which can lead to electrolyte imbalances.
- 3. Know Your Family History: If there’s a family history of sudden cardiac death or known cases of Long QT Syndrome, consider genetic testing and regular cardiac screenings.
- 4. Avoid Triggers: For those diagnosed with Long QT Syndrome, it’s essential to recognize and avoid specific triggers. This might include sudden loud noises for some or intense physical exertion for others.
- 5. Stay Informed: New research and findings emerge regularly. Stay updated on the latest information regarding TdP and its risk factors.
Chapter 12: Case Studies: Real-life Scenarios
Case studies provide valuable insights into the complexities of TdP, offering a real-world perspective on its presentation, diagnosis, and management.
- Case 1: The Unexpected Reaction Sarah, a 28-year-old woman, was prescribed a common antibiotic for a respiratory infection. Days into her treatment, she experienced sudden fainting spells. An ECG revealed a prolonged QT interval, and she was diagnosed with drug-induced TdP.
- Case 2: The Genetic Link John, a 35-year-old athlete, had a family history of sudden cardiac deaths. After experiencing palpitations during a workout, he underwent genetic testing and was diagnosed with Long QT Syndrome, putting him at risk for TdP.
- Case 3: The Silent Threat Emma, a 42-year-old teacher, had no apparent symptoms but decided to have a routine health check-up. Her ECG showed a prolonged QT interval, and further investigations revealed an underlying electrolyte imbalance as the cause.
Chapter 13: The Psychological Impact of Torsades de Pointes
Being diagnosed with a condition like TdP can have profound psychological implications. The constant fear of a life-threatening arrhythmia and lifestyle modifications and medical interventions can lead to anxiety, depression, and reduced quality of life.
- Anxiety and Fear: The unpredictability of TdP episodes can lead to constant pressure. Patients might fear physical exertion, specific emotional triggers, or even sleep.
- Depression: The limitations imposed by the condition, coupled with its potential severity, can lead to feelings of sadness, hopelessness, and depression.
- Coping Mechanisms: It’s essential to develop coping strategies. This might include counselling, joining support groups, practising relaxation techniques, or seeking psychiatric interventions.
- Educating Loved Ones: Ensuring that family and friends understand the condition can provide a supportive environment for the patient.
Chapter 14: Research and Future Directions
- Cardiology is ever-evolving, with continuous research shedding light on Torsades de Pointes (TdP) ‘s intricacies and management. This chapter delves into the latest research findings and the potential future directions in understanding and treating TdP.
- 1. Genetic Insights: With advancements in genetic testing, researchers are identifying more genes associated with Long QT Syndrome. This not only aids in diagnosis but also in understanding the underlying mechanisms of TdP.
- 2. Drug Development: Efforts are underway to develop drugs that can effectively treat TdP without causing additional cardiac side effects. This includes medicines that stabilize the heart’s electrical activity without affecting the QT interval.
- 3. Wearable Technology: The rise of wearable health tech, like smartwatches with ECG capabilities, offers promise in early detection and monitoring of QT prolongation and potential TdP episodes.
- 4. Personalized Medicine: Recognizing that every patient is unique, there’s a push towards personalized medicine. This involves tailoring treatment based on an individual’s genetic makeup, lifestyle, and other factors.
- 5. Improved Risk Stratification: Research is focused on better identifying those at the highest risk of developing TdP, allowing for more targeted interventions.
Chapter 15: A Holistic Approach to Heart Health
While understanding and managing TdP is crucial, adopting a holistic approach to heart health is equally important. This encompasses medical interventions, lifestyle modifications, mental well-being, and preventive measures.
- 1. Diet and Nutrition: A balanced diet, rich in whole grains, fruits, vegetables, lean proteins, and healthy fats, can support overall heart health. Ensuring adequate intake of potassium and magnesium can also help prevent TdP.
- 2. Physical Activity: Regular exercise strengthens the heart and improves cardiovascular health. However, for those at risk of TdP, it’s essential to consult with a healthcare provider to determine safe exertion levels.
- 3. Stress Management: Chronic stress can adversely affect the heart. Techniques like meditation, deep breathing exercises, and yoga can help manage and reduce stress.
- 4. Regular Check-ups: Routine medical check-ups, including ECGs, can help detect and address potential issues before they become severe.
- 5. Mental Well-being: As discussed in Chapter 13, the psychological impact of TdP can be profound. Seeking support through counselling, support groups, or other means is crucial for mental well-being.
- 6. Education and Awareness: Staying informed about one’s condition, potential triggers, and the latest research findings can empower patients to take charge of their health.
In conclusion, while a complex and potentially life-threatening condition, Torsades de Pointes can be managed and treated with the proper knowledge and interventions. This aims to provide a comprehensive overview, from understanding the basics of the heart’s electrical system to the latest research findings. Whether you’re a healthcare professional, a patient, or someone keen to learn, it’s hoped that this guide offers valuable insights into the spiral dance of the heart.
Disclaimer: This book and its content are intended for informational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or another qualified health provider with any questions you may have regarding a medical condition.




